Appointments Call
(02) 9126 8963
Appointments Call
(02) 9126 8963
It largely depends on the type of surgery and so we need to understand what the surgery entails.
In the case of sleeve surgery a significant portion of the stomach is removed. On the other hand, the gastric band doesn’t have staples but rather has a ring around it. Meanwhile, the bypass uses staples and is also connected to the bowel.
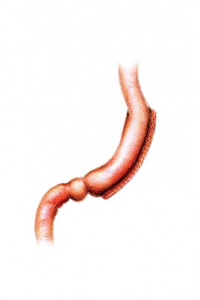

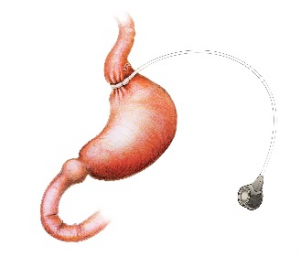

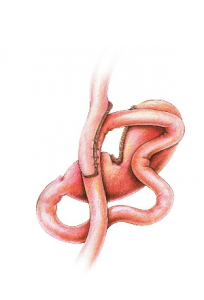

Substantial risk are rare but include potential infection, leakage at the staple line, bleeding needing a transfusion or return to the operating room, or blood clot. These more severe complications have a likelihood of about 1 to 2%, making them relatively uncommon.
Another concern associated with the sleeve gastrectomy is reflux. While it’s rare for it to be a grave issue, it can sometimes become bothersome, necessitating medication.
There are inherent risks with anesthesia. While they are minimal, there’s a possibility of allergic reactions to a medication, or developing a blood clot, similar to the risks posed by long flights.
Furthermore, one should consider long-term nutritional risks. Patients are often advised to take multivitamins and maintain a well-balanced diet. Some individuals might be slightly malnourished even before the surgery. For instance, their vitamin D levels could be low. However, as long as patients adhere to taking multivitamins, nutritional deficiencies are uncommon. The gastric bypass, which bypasses about a metre and a half of the bowel, might increase the risk of iron deficiency.
Longer term risks for the gastric bypass include small possibility, around 5%, of leading to an ulcer in the stomach or a twist in the bowel. These risks aren’t present for the sleeve gastrectomy which makes it appealing for this reason. For the gastric band, the primary concern usually relates to its tolerance. At times, the stomach might shift in relation to the band (slipped gastric band), which can necessitate corrective surgery